
More than a billion people worldwide live with migraine, yet most still confuse it with an ordinary headache. We look at what current research says — and what actually helps.
Migraine is one of the most widespread neurological disorders in the world. According to the World Health Organization, it affects more than 1 billion people, and for many patients it is one of the leading causes of temporary disability. Despite this, migraine is routinely dismissed as a regular headache — a misconception that significantly delays proper diagnosis and treatment.
What the science confirms
Migraine is a neurological condition — not psychosomatic, and not simply stress. Research shows that during an attack the trigeminal nerve becomes activated, and blood levels of the neuropeptide CGRP spike sharply. CGRP amplifies pain signaling and promotes inflammation, and is now a key target for modern migraine medications.
How to recognize an attack
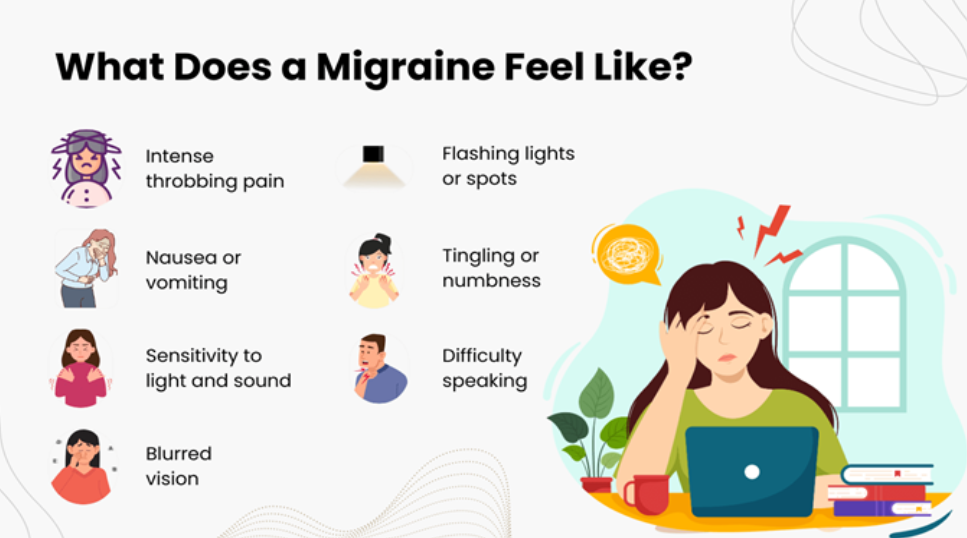
A migraine attack differs from ordinary headache in several distinct ways. The pain is typically throbbing and concentrated on one side of the head, accompanied by heightened sensitivity to light and sound, and often by nausea or vomiting. Physical movement tends to make symptoms worse. An attack can last anywhere from 4 hours to 72 hours.
Around 20–30% of patients experience an aura before the pain begins — visual or sensory disturbances such as flashes of light, zigzag lines, temporary blind spots, or tingling in the hands. An aura typically lasts between 20 and 60 minutes.
What triggers an attack
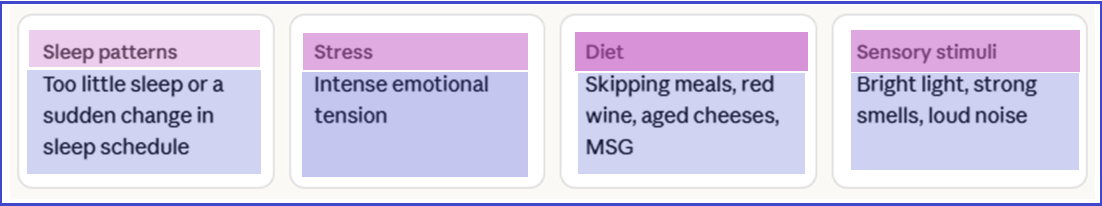
Specialists refer to these precipitating factors as triggers. Crucially, triggers are highly individual — what provokes an attack in one person may be completely harmless for another.
Stopping an attack entirely is not always possible, but its severity can be reduced. Resting in a quiet, darkened room, applying a cold compress to the forehead or back of the neck, and drinking enough water are the first steps recommended by clinicians.
When prescribed by a doctor, pain relievers, anti-inflammatory drugs, and triptans — a class of medications developed specifically for migraine — may be used. For patients with frequent attacks, a neurologist may recommend preventive therapy to reduce their overall frequency.
When to seek emergency care
Seek immediate medical attention if a headache comes on suddenly and is the worst you have ever experienced, if it is accompanied by speech problems, vision loss, or loss of coordination, if it lasts more than three days, or if the character of your usual headache has changed significantly. These signs may indicate a more serious underlying condition.
Can the frequency of attacks be reduced?
Yes — and lifestyle plays a central role. A consistent sleep schedule, regular meals without long gaps, adequate hydration, and moderate physical activity all help reduce the likelihood of attacks. Doctors also frequently recommend keeping a migraine diary: recording the date, duration, and possible triggers of each episode helps identify personal patterns over time.
Sources
1.World Health Organization — Headache disorders fact sheet
2.American Migraine Foundation — Migraine Triggers
3.National Institute of Neurological Disorders and Stroke — Migraine Information Page
4.Mayo Clinic — Migraine: Symptoms and causes
5.Cleveland Clinic — Migraine: Symptoms, Causes and Treatment




















